The genetic mutation arose 7,300 years ago in just one person in West Africa, scientists reported on Thursday. Its advantage: a shield against rampant malaria.
Thousands of years ago, a special child was born in the Sahara. At the time, this was not a desert; it was a green belt of savannas, woodlands, lakes and rivers. Bands of hunter-gatherers thrived there, catching fish and spearing hippos.
A genetic mutation had altered the child’s hemoglobin, the molecule in red blood cells that ferries oxygen through the body. It was not harmful; there are two copies of every gene, and the child’s other hemoglobin gene was normal. The child survived, had a family and passed down the mutation to future generations.
As the greenery turned to desert, the descendants of the hunter-gatherers became cattle-herders and farmers, and moved to other parts of Africa. The mutation endured over generations, and for good reason. People who carried one mutated gene were protected against one of the biggest threats to humans in the region: malaria.
There was just one problem with this genetic advantage: From time to time, two descendants of that child would meet and start a family. Some of their children inherited two copies of the mutant hemoglobin gene instead of one.
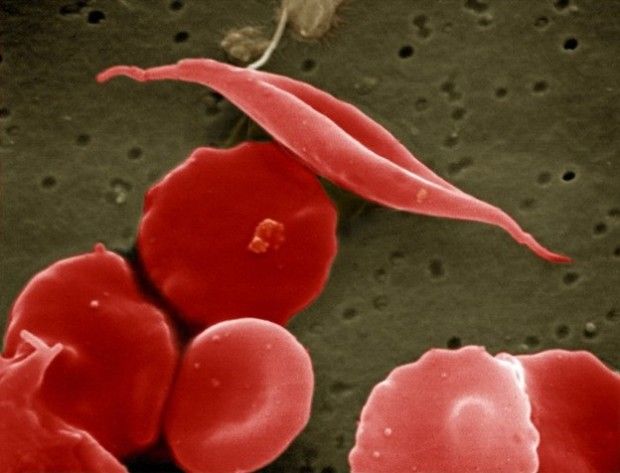
These children could no longer produce normal hemoglobin. As a result, their red cells became defective and clogged their blood vessels. The condition, now known as sickle cell anemia, leads to extreme pain, difficulty with breathing, kidney failure and even strokes.
In early human societies, most children with sickle cell anemia likely died by age 5. Yet the protection afforded by a single copy of the sickle cell mutation against malaria kept fueling its spread.
Today, over 250 generations later, the sickle cell mutation has been inherited by millions of people. While the majority of carriers live in Africa, many others live in southern Europe, the Near East and India. Those carriers have about 300,000 children each year with sickle cell anemia.

A colored scanning electron micrograph of a female Anopheles gambiae mosquito, a carrier of malaria. People with the sickle cell mutation are more resistant to malaria.
How humans got the sickle cell mutation is a sprawling saga that emerges from new research carried out at the Center for Research on Genomics and Global Health, part of the National Institutes of Health, by Daniel Shriner, a staff scientist, and Charles N. Rotimi, the center’s director. Their study was published on Thursday in the American Journal of Human Genetics.
Dr. Shriner and Dr. Rotimi analyzed the genomes of nearly 3,000 people to reconstruct the genetic history of the disease. They conclude that the mutation arose roughly 7,300 years ago in West Africa.
Later, migrants spread the mutation across much of Africa and then to other parts of the world. Wherever people suffered from malaria, the protective gene thrived — but brought sickle cell anemia with it.
Today, sickle cell anemia remains a heavy burden on public health. In many poor countries, most children with the disease still die young. In the United States, the average life span of sufferers has been extended into the early 40s.
Dr. Rotimi said that an improved understanding of the history of sickle cell anemia could lead to better medical care. It might allow researchers to predict who will suffer severe symptoms and who will only experience mild ones.
“It would definitely help physicians to treat patients at a global level,” he said.
Doctors in the United States first noticed sickle cell anemia in the early 1900s. The disease got its name from the way it changed the shape of red blood cells from healthy disks to abnormal curves.
Most cases turned up in African-Americans, doctors found. But 8 percent of African-Americans had at least some sickle-shaped blood cells, even though the vast majority had no symptoms at all.
By 1950, researchers had resolved this paradox, discovering the difference between carrying one mutated copy of the hemoglobin gene and carrying two copies. By then it had also become clear that sickle cell anemia was not unique to the United States.
In Africa, researchers found sickle-shaped red blood cells in people across a broad belt, from Nigeria in West Africa to Tanzania in the east. The cells also turned up at high rates in people in parts of the Near East and India, and in southern European countries such as Greece.
Genetically speaking, this made no sense. Because inheriting two copies of the gene is so deadly, the mutation should have become rarer with passing generations, not more common.
In 1954, a South African-born geneticist named Anthony C. Allison observed that people in Uganda who carried a copy of the sickle cell mutation suffered fewer malaria infections than people with normal hemoglobin.
Later research confirmed Dr. Allison’s finding. The sickle cell mutation seemed to defend against malaria by starving the single-celled parasite that causes the disease. The parasite feeds on hemoglobin, and so it’s possible that it can’t grow on the sickle cell version of the molecule.